Request for Change
Change Request OMB-0920-1281 STEADI Cost Effectiveness.docx
Evaluation of CDC’s STEADI Older Adult Fall Prevention Initiative in a Primary Care Setting
Request for Change
OMB: 0920-1281
Evaluation of CDC’s STEADI Older Adult Fall Prevention Initiative in a Primary Care Setting (OMB no. 0920-1281 exp. date 01/31/2023)
Proposed Changes: Change request to modify incentives for respondents completing baseline and follow up surveys
Justification
This Non-Substantive change request is related to the ICR entitled, “Evaluation of CDC’s STEADI Older Adult Fall Prevention Initiative in a Primary Care Setting,” OMB control number 0920-1281.
This Non-Substantive change request is to modify the incentive provided for the baseline and follow-up patient surveys and does not include changes to the currently approved burden and/or costs to the public.
Project Description
Falls are the leading cause of both fatal and non-fatal injuries among older adults. The economic consequences of falls are significant and growing, and falls cost the U.S. $50 billion each year.1 Falls are preventable by targeting modifiable fall risk factors. The Stopping Elderly Accidents, Deaths, and Injuries (STEADI) Initiative, developed by the Centers for Disease Control and Prevention (CDC) and based on the American and British Geriatrics Societies guidelines, provides tools and resources to healthcare providers and older adults to prevent unintentional falls.2,3
CDCD received approval from OMB for the ICR “Evaluation of CDC’s STEADI Older Adult Fall Prevention Initiative in a Primary Care Setting” (OMB no. 0920-1281). The goal of this study is to evaluate the STEADI initiative in a primary care setting. Data from older adults is collected by administering patient surveys (1 baseline and 3 follow-up surveys) to identify the number of falls patients have after entering the study and the fall prevention behaviors practiced. A pre-survey incentive of 6 first class stamps (equivalent to $3.48) was approved by OMB for this ICR. Due to the COVID-19 pandemic, many non-acute visits have taken place via telemedicine in the selected healthcare system. Patient recruitment into the study for the baseline patient survey, and follow-up patient surveys were previously modified to appropriately capture information in a telemedicine environment (see approval attachments 1 and 2).
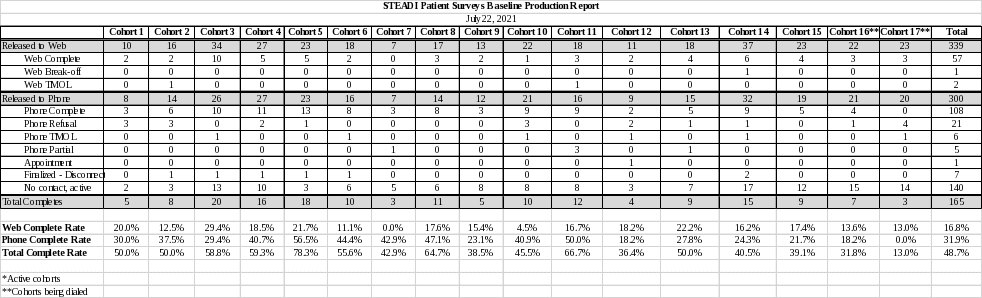
However, survey response rates are low (Table 1) which may impact the validity of the study. Previous research indicates that the inclusion of pre-survey incentives will improve the survey sample and response rates. A previous study showed that a cash incentive increased response rates across the board in a survey of Medicaid recipients.5 Other studies have shown that incentives increase participation of respondents typically under-represented in surveys such as those with low education levels,6 racial/ethnic minorities, and low-income households.7 This change request is to request approve to change into $2 cash as a pre-survey incentive or to approve additional items as pre-survey incentive (i.e. Agenda booklet and/or microfiber glasses cleaning cloth).
Proposed Changes
OMB previously approved the ICR “Evaluation of CDC’s STEADI Older Adult Fall Prevention Initiative in a Primary Care Setting” (OMB no. 0920-1281 exp. date 01/31/2023). In this ICR, NCIPC was approved to collect data from patients using the baseline and follow-up patient surveys (attachments 1 and 2) with a survey incentive of postage stamps.
In the telemedicine environment, patient recruitment and enrollment into the study is lower than originally expected. These low recruitment rates are also compounded with low patient participation in the post visit surveys.
A pre-survey incentive would likely motivate participation in baseline and follow up surveys.
Previously, six first class postage stamps (equivalent to $3.48) were approved to be provided to patients for each survey.
This request is to approve the change into $2 cash as a pre-survey incentive.
If the cash incentive is not allowed, the request is to approve additional items as pre-survey incentive (Agenda booklet and/or microfiber glasses cleaning cloth).
Change to Burden and/or Cost
This non-substantive change request does not include changes to the currently approved burden and/or costs to the public.
References
Florence CS, Bergen G, Atherly A, Burns ER, Stevens JA, Drake C. Medical Costs of Fatal and Nonfatal Falls in Older Adults. Journal of the American Geriatrics Society, 2018 March, DOI:10.1111/jgs.15304
Summary of the Updated American Geriatrics Society/British Geriatrics Society clinical practice guideline for prevention of falls in older persons. J Am Geriatr Soc. Jan 2011;59(1):148-57. doi:10.1111/j.1532-5415.2010.03234.
Johnston YA, Bergen G, Bauer M, Parker E, Wentworth L, et al. Implementation of the Stopping Elderly Accidents, Deaths, and Injuries Initiative in Primary Care: An Outcome Evaluation, The Gerontologist. Dec. 2019; 59 (6): 1182–1191. https://doi.org/10.1093/geront/gny101
Beebe TJ, Davern ME, McAlpine DD, Call KT, Rockwood TH. (2005) Increasing response rates in a survey of Medicaid enrollees: the effect of a prepaid monetary incentive and mixed modes (mail and telephone). Med Care. 2005 Apr;43(4):411-4.
Singer E, van Hoewyk J, Maher MP. Experiments with incentives in telephone surveys. Public Opin Q. 2000; 64:171–188.
Mack S, Huggins V, Keathley D, Sudukehi M. Do Monetary Incentives Improve Response Rates in the Survey of Income and Program Participation? U.S. Bureau of the Census, Demographic Statistical Methods Division, Washington D.C. 20233. Available at: http://www.amstat.org/sections/srms/Proceedings/papers/1998_089.pdf
| File Type | application/vnd.openxmlformats-officedocument.wordprocessingml.document |
| File Title | Change Request Guidance |
| Author | jahlani akil |
| File Modified | 0000-00-00 |
| File Created | 2022-02-12 |
© 2026 OMB.report | Privacy Policy